.jpg)
1.UNDERSTANDING THE PATIENT, PATIENTS VISUAL SYSTEM AND VISUAL ENVIRONMENT
HISTORY TAKING:
History taking forms the basic foundation for all medical examination. A well taken history may lead to make correct diagnosis. The basis of true history taking is good and direct communication between patient and the practitioner.
VISUAL ACUITY TEST:
Visual acuity is the fundamental characteristic of the visual system and is the prime determinant of any regime that aims to improve visual and therefore occupational performance.
2.CLINICAL REFRACTION:
Correction of Refractive Error:

True objective of the refraction is to provide the patient clear and comfortable vision to which he adapts quickly and which allows him to work for a longer period of time without any symptoms.
Subjective Refraction:

1. Subjective refraction is initiated by selecting an initial trials lens which may be based on the following factors-
-->Current lens prescription of the patient.
--> A set of lenses you decide based on your initial data collection
--> It may be the results of auto refractometer or retinoscope.
2. It is prudent to check axis first, and then the amount of cylinder correction and finally spherical correction needed.
3. Measure the vertex distance in high refractive error above -5.00D for myopes and above +4.00D in hyperopes as the effect of prescribed minus power will reduce if vertex distance increases and it will increase with plus lens.
4. Do not exceed spherical by 0.75D, cylinder by 0.50D and axis by 10o.
Refinements:
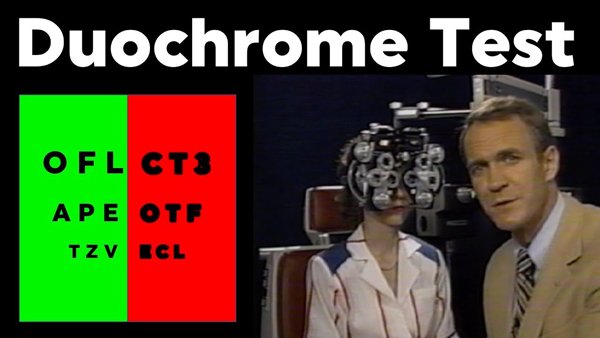
• Duochrome test for spherical end point.
• Binocular balancing.
Duochrome test for spherical end point is performed to refine the spherical correction.
Binocular balancing is performed to equalize the stimulus to the most common procedure which is normally used:
• Alternate occlusion test.
Enhancements:

Traditionally, refraction is done at a distance for 20 feet and for near at a distance of 40 cm. One of the most important factors for computer users is the allowance for the distance at which the monitor is placed.

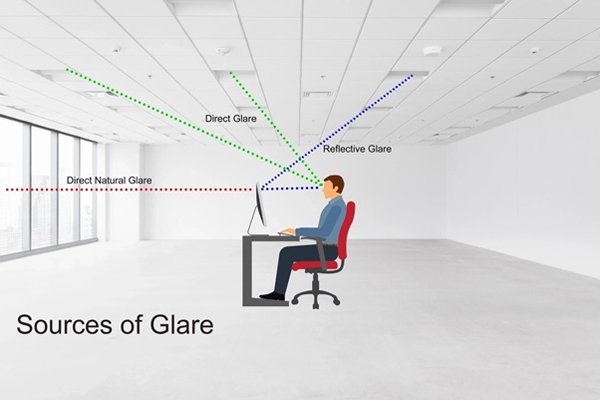
Checking the presence of Glare:

Use luminance meter to assess the amount of luminance. We can asses the over illumination.
Solutions to Discomfort Glare:
Over-illumination, unequal distribution of illumination, improper light fitting auxillary light fitting-all may cause discomfort glare.
Check the screen brightness:
The brightness of the screen should be adjusted to match the brightness of the visual objects that immediately surround it.

Management:
• Remove the source of the reflections.
• Tilt or rotate the display to some other direction.
ROLE OF ANTI REFLECTION SPECTACLE LENSES:

Antireflection coating on spectacle lenses are very often advised to the computer workers, but it is a fact that they do not affect reflections in the computer displays and also they do not offer any advantage other than what they have in general.
WHY WE NEED BLUE LIGHT LENSES OR GLASSES?
• Blue light is everywhere - While manmade sources of blue light include fluorescent and LED lighting, flat-screen televisions, and the display screens of computers, electronic notebooks, smartphones and other digital devices; our main source of blue light is the sun, and we are most exposed to it when we are outdoors during daylight hours. This is where the most damage occurs and our children are also vulnerable to it since they are more likely to spend a significant amount of time outdoors whether at school or in the playing field.
• Natural blockers are ineffective - While the cornea and lens of the eye are effective at blocking UV rays from reaching our light-sensitive retinas, almost all visible blue light passes through these barriers, which could reach and damage the delicate retina.
It contributes to digital eye strain – While this is less dangerous than the effects of the blue light generated by the sun, digital eye strain is something we are all at risk of. Most people spend at least 12 hours a day in front of a screen, though it takes as little as two hours to cause digital eye strain. Dry eyes, eye strain, headaches and tired eyes are all common results of staring at screens for too long. Blue light exposure from computers and other digital devices can be reduced with special computer glasses.
Best Blue-Light-Blocking Glasses

Blue-light-blocking capability: All light is measured in nanometers (nm), and blue-light wavelengths that can have the most impact on your melatonin levels (and thus affect your sleep) range from 400 to 500 nm. Blue-light-blocking glasses work by absorbing those wavelengths to stop them from reaching your eyes. (Note that despite emitting blue light, most consumer tech is not harmful, and there is no scientific evidence that digital devices can damage your eyes.)
Many blue-light-blocking glasses have an orange or yellow tint that is supposed to absorb the blue light while allowing other light to pass through. Generally, the darker the lenses on a pair of blue-light-blocking glasses, the more blue light is blocked. While there are clear or less obviously tinted blue-light-blocking lenses, they won’t filter as much blue light as darker options.
Anti-glare coating: Blue-light-blocking glasses may have anti-glare coating, which decreases the amount of light reflecting from your glasses to further reduce eye strain and make them more comfortable to use. This is especially handy during video calls where people are going to be looking at you for long periods of time.
Since the best time to use blue-light-blocking glasses is in the evening or right before bed (which means you’re unlikely to wear them out of the house), the function-first, orange-tinted design of many pairs will suffice for a lot of people. But if you hate the look of the orange tint, we’ve found some blue-light-blocking glasses with almost clear lenses — as long as you’re willing to sacrifice some of their light-filtering capabilities.

Frame material: There are different frame materials to choose from including wire, plastic, and acetate, depending on how stylish you want to get. If you don’t already wear prescription or reading glasses, any pair of blue-light-blocking glasses will be easy to pick up and use. But if you do, you’ll want to look for either a prescription pair, reading glasses with blue-light-blocking capabilities, or something that will clip onto or fit over the top of your existing glasses.
Prescription requirement: While you don’t need a doctor’s prescription to get a pair of these glasses, some lenses and frames are compatible with prescription lenses, so you won’t have to switch between the two and sacrifice vision for comfort. We’ve noted which are simply nonprescription and which can work with your existing or new prescriptions.
Where is the best place to buy blue light glasses?

Please click here to have a bird's eye view of optical: DRSURESH EYE OPTICALS.
Presbyopia and Computer Use:
Progressive Addition Lenses:
.jpg)
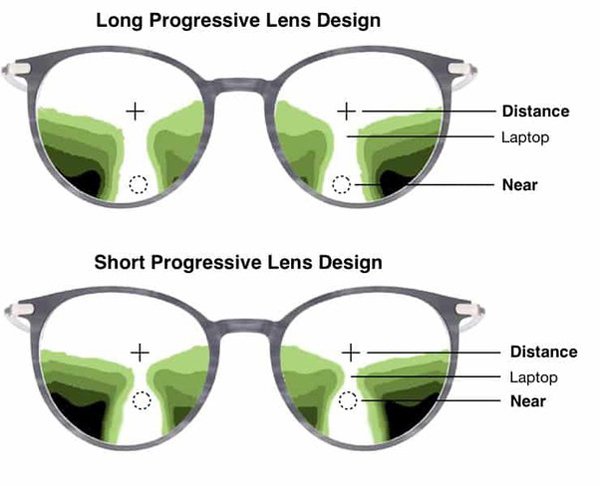
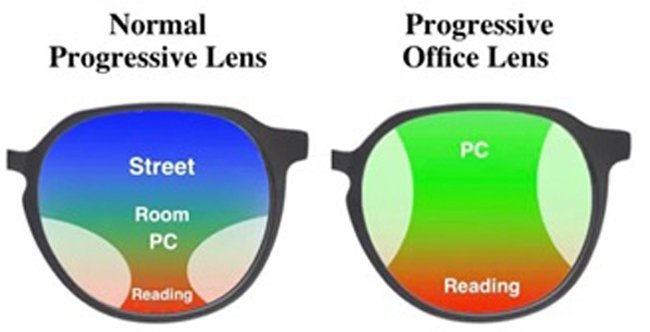
Progressive addition lenses are another common lens design used to correct presbyopia. These lenses are characterized by a smooth continuous change of power across the lens surface, but with undesired aberrations at the lower periphery on either side. The smooth change in the power across the lens surface provides the user a region with intermediate power. It is for this reason they are most commonly prescribed for computer use.
3.ASSESSMENT OF VISUAL SYSTEM:
ASSESSMENT OF CONVERGENCE - RAF (Royal Air Force Rule) & Accommodation:


RAF Rule (Royal Air Force Rule) provides a binocular gauge to measure Objective and Subjective Convergence as well as Accommodation in 1 mm increments. The RAF Rule consists of a 50 cm long rule with a slider holding a rotating four-sided cube. Each side has a different target. The first has a vertical line with a central dot for convergence fixation. The others provide a limited number of lines of near reading examples.
This instrument is used for determining the objective and subjective convergence points, examining the accommodation and determining the master eye. The RAF Rule is useful for both diagnosis and treatment.
Treatment :
The first line of treatment for any anomaly of accommodative function is correction of refraction error. Low plus lens in the range of +0.50D to +1.00D over the distance correction is very effective treatment.
ASSESSMENT OF BINOCULAR VISION:
40 cm is the standard distance at which the near vision is assessed. The computer monitor is usually at a distance of 50-60cm. A diagnosed binocular vision problem at 40 cm almost certainly indicates a binocular vision problem at computer screen.
1. Stereopsis Test

There are two types of common clinical tests for stereopsis and stereoacuity: random dot stereotests and contour stereotests. Random-dot stereopsis tests use pictures of stereo figures that are embedded in a background of random dots
SLIT LAMP EXAMINATION (SLE):

Most of the time, your doctor can diagnose conjunctivitis by using a slit lamp—an instrument that consists of a microscope and a high-energy beam of light. During a slit-lamp exam, your ophthalmologist shines a thin beam of light into your eye. This beam allows your doctor to examine the entire eye, including the conjunctiva; the sclera, or the white of the eye; the iris; and the cornea.
For a more detailed look at the eye, your doctor may put a drop of a yellow dye called fluorescein into your eye, which allows him or her to see any damage to the surface of the eye.
NON CONTACT TONOMETER:

A non-contact tonometer uses a small puff of air (which is why it's many times referred to as the "puff test") to measure an eye's pressure.
FUNDUS CAMERA:
.jpg)
This is done to detect any optic nerve damage.
Eye Movement Disorder and its Management:
WHAT IS LATENT SQUINT
It’s a condition where the eyes have a tendency to become misaligned when not being used e.g. when the eye is covered.
HOW DOES THIS HAPPEN
• This correction of tendency to deviate is corrected by continuous effort of binocular fusion By the brain.(week 4)
• This is done by combined use of the sensory and motor systems.
• The motor system acts to fixate both eyes at specific object.
• Any offset is detected visually(and the motor system corrects it)
• Heterophoria only occurs during dissociation of the left eye and right eye (absent fusion).
• If you cover one eye (with your hand) you remove he sensory information about the eye’s position in the orbit.
• Without this, there is no stimulus to binocular fusion.
Symptoms:
• Symptoms of muscular fatigue:

– Headache.
– Asthenopia (eyestrain).
– Photophobia (increased sensitivity to light).
– Difficulty in changing focus from near to distance and vice versa.
• Symptoms due to failure in maintaining binocular single vision (BSV): These are
– Blurring of vision.
– Crowding of words while reading.
– Difficulty with stereopsis.
– Intermittent diplopia.
– Intermittent squint without diplopia.
• Symptoms due to defective postural sensations: These causes
– Problem in judging distances and positions, especially of objects in motion.
Clinical types of Latent squint:
Exophoria: It is characterised by a tendency of the eyes to diverge.
Esophoria: It is characterised by a tendency of the eyes to deviate inwards.
2. Cover Test (fixation, phorias)
3. Ocular Movements:
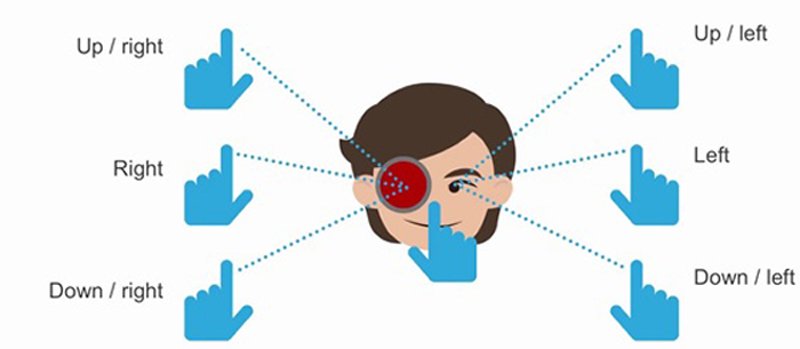
Maddox wing:

MANAGEMENT
Treatment:

Like any other treatment for binocular vision disorder, prescribing for any uncorrected refractive error is the first consideration.
Lesser degrees of heterophoria without any symptoms require no treatment except for correction of refractive error, if present.
Medical therapy:
• Esophoria management:

– Full correction of the refractive error is given to the patient when refraction shows significant amount of hypermetropia
– Patients symptomatic esophoria without hypermetropia may be treated with miotics or bifocal glasses.
– Base-out prisms for visual comfort in patients with non-accommodative esophoria.. This does not correct underlying cause of latent deviation. It is used mainly in elderly patients with symptomatic esophoria who do not respond to orthoptic treatment.
• Exophoria management:
– Patients without asthenopia do not require any treatment.
– Significant refractive errors, especially anisometropia, aniseikonia, aphakia, intraocular lens (IOL) with wrong power (pseudophakia), and astigmatism, should be treated to produce sharp retinal images which increase stimulus to fuse. Hypermetropia of less than 2 Dioptres may be left uncorrected in children, though in older patients this needs to be corrected to avoid asthenopia. Presbyopia patients are given the weakest bifocal lenses which provide comfortable near vision. Half of exodeviation may be treated with base-in prisms for near vision. Myopic errors are fully corrected.
– Minus lenses may decrease exodeviation in patients with high AC/A ratio.
– In younger children with convergence insufficiency exodeviation, minus lenses as lower segment bifocals may be tried, as a temporary measure. In divergence excess exodeviation, minus lenses as upper segment bifocals may be tried.
III. Miotic drugs:
Miotic drugs may be useful in near esophoria due to high AC/A ratio. These facilitate peripheral accommodation so that less than normal innervation is required and consequently less than normal accommodative convergence occurs.
Surgical therapy:
This is indicated in patients with intermittent exotropia who show signs of worsening in the form of
• Exotropia lasts for more than 50% of the waking hours.
• There are symptoms of asthenopia or diplopia.
• Patient develops abnormal retinal correspondence or suppression.
• There is decrease in stereo-acuity.
• There is development of secondary convergence insufficiency.
• There is increase in deviation.
4.OTHER BINOCULAR TESTS:
4. Worth 4D Test:

Treatment:
Once the diagnosis of binocular vision anomalies is established, it is relatively easier to plan the sequence of treatment management. Lenses, prisms, mirrors and vision training procedures.
Plus lens induces base in effect and minus lens include base out effect.
• Contrast sensitivity Test

Pelli-Robson contrast sensitivity chart.
The most common contrast sensitivity test is the Pelli-Robson contrast sensitivity chart. This test is a chart with different capital letters organized in horizontal lines. The contrast decreases with each line. The person will move down the chart to determine the least level of contrast they can see.
• Amsler
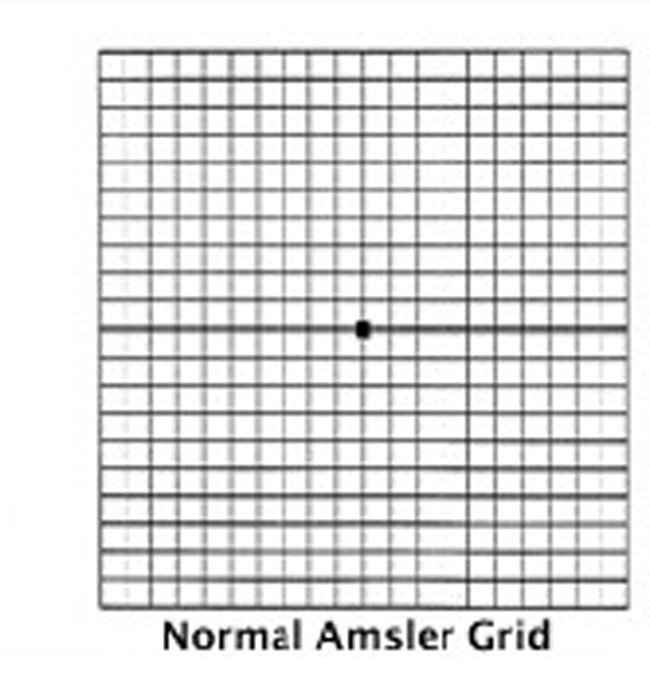
The Amsler grid can help detect early signs of retinal disease and monitor changes in vision after diagnosis.
• Colour Vision Test

Color plate test
This is the most common type of color blindness test. Your eye doctor will ask you to look at an image made up of colored dots with a differently colored number or shape in the middle. If the shape blends into the background and you can't see it, you may have a type of color blindness.
• Blink rate Assessment

The normal blink rate for humans is between 12 and 15 blinks per minute (bpm). Screen use has been associated with decreased blink rate and increased percentage of incomplete blinks, however, little is known about the effects of videogaming on blink rate.
The blink rate is measured in blink/min and corresponds to the number of blinks occurring during a certain period. The blink duration is measured in seconds and corresponds to time difference between the start and end points of a blink.
COMPUTER USE AND DRY EYE:
• Dry Eye Test.
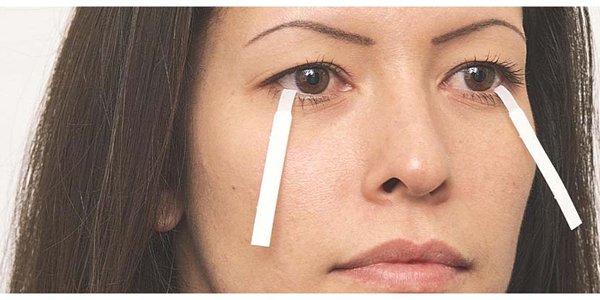
Schirmer Test:
The Shirmers test is used to check the amount of tears in your eyes.
Treatment of Ocular Conditions:
Tear replacement should be the first step and can be done with artificial tears that exist in many pharmaceutical presentations with or without preservatives.
Patient Counselling:

• Avoid smoking
• Reduce caffeine intake
• Increase the amount of water they drink
• May be asked to consult his physician to alter the medications that could be aggravating the dry eye symptoms.
• The patient may be advised to blink more frequently.
• He may also be advised to take an occasional two minute break, look into the distance, and concentrate on blinking.
PLEASE CLICK HERE FOR MORE DETAILS ABOUT :COMPUTER VISION SYNDROME -I SYMPTOMS
PLEASE CLICK HERE FOR MORE DETAILS ABOUT: COMPUTER VISION SYNDROME- III WORKING ENVIRONMENT ASSESSMENT.
.jpg)
1.jpg)
{{r.reply}}
Your comment was submitted for review. It will start display once it was approved by Admin
Comments